Congratulations on completing the first phase of the low FODMAP diet! By now, your gut is likely feeling a lot more settled, and you’ve seen firsthand how low FODMAP foods can help reduce your symptoms. That’s a huge achievement—and it means you’re ready for the next important step: the FODMAP reintroduction phase. This is where you begin to reclaim your food freedom and pinpoint exactly which FODMAPs your body can tolerate, and which ones may be involved in symptoms.
If it still feels like your gut has a vendetta against you, then it’s time to talk to a dietitian and look at some troubleshooting strategies before you attempt the FODMAP reintroduction phase.
Please note that this article does not replace the advice or expertise of a registered dietitian, who specialises in the low FODMAP diet. A dietitian can help tailor FODMAP reintroduction challenges to suit your lifestyle and medical needs. If you are unable to access a dietitian, then you can get expert reintroduction support through the FODMAP Made Easy program.
This Article Will Cover:
- What is the FODMAP reintroduction phase?
- Why do the FODMAP Reintroduction phase if you feel good?
- What to do when you find a problem food
- Your FODMAP Reintroduction Guide:
- How To Get FODMAP Reintroduction Help
- Common FODMAP Reintroduction Mistakes
Let’s get started.
What is the FODMAP reintroduction phase?
The FODMAP reintroduction phase (also known as the FODMAP challenge phase) is the second stage of the low FODMAP diet. The main goal of this phase is to figure out which types of FODMAPs are involved your gut symptoms—and which ones your body can handle just fine.
Let’s back up for a second: FODMAP stands for Fermentable Oligosaccharides, Disaccharides, Monosaccharides And Polyols. These are different types of fermentable sugars that can cause digestive issues in people with irritable bowel syndrome.
During the reintroduction phase, you’ll test each FODMAP group one at a time through a process called a food challenge. Here’s how it works:
- Each week, you choose one FODMAP group to test (like lactose or fructose).
- You’ll eat a specific challenge food from that FODMAP group over three days, gradually increasing the amount each day. Note, this does not have to be 3 days in a row.
- During and after the challenge, you’ll track your gut symptoms—things like bloating, gas, stomach pain, or changes in your bowel habits.
This process helps you understand your personal tolerance to each FODMAP group:
- Some groups may not impact your digestion at all, and you can enjoy foods from that group freely.
- Others might be tolerated well in certain amounts.
- And you may decide to be watchful of a few FODMAPs most of the time to keep your gut symptoms settled.
SUMMARY
The FODMAP reintroduction phase can also be called the FODMAP challenge phase. This phase involves a series of food challenges that help you identify which of the FODMAP groups are involved in your gut symptoms.

Why do the FODMAP Reintroduction Phase if you feel good?
If your gut symptoms have finally settled and you are feeling amazing on the low FODMAP diet, you might be wondering:
“Why mess with a good thing? Shouldn’t I just stick with what’s working?”
It’s a totally understandable thought! But while the low FODMAP diet can be life-changing in the short term, it’s not meant to be a long-term solution. The good news is that, on average, most people only find that 2.5 FODMAP groups are problematic. That’s where the FODMAP reintroduction phase comes in—and it’s actually one of the most important parts of the whole process.
Here’s why:
-
You Need to Know Your which FODMAPs impact your gut symptoms
Everyone with IBS is different. Some people find fructose problematic, others to lactose, and some only to large amounts of Fructans.
By doing a structured reintroduction, you’ll learn exactly which FODMAP groups are involved in symptoms and which ones you can enjoy without any trouble. This knowledge gives you the confidence to eat with less anxiety and more freedom.
-
FODMAPs Are Actually Good for Your Gut
It might sound surprising, but many high FODMAP foods are actually great for gut health. That’s because they feed your healthy gut bacteria—functioning like prebiotics, which help keep your microbiome balanced and thriving.
If you avoid all FODMAPs for too long, it can potentially have a negative impact on your gut bacteria and overall digestive health.
-
Staying Low FODMAP Forever Is Hard And Unnecessary
Let’s face it: the low FODMAP diet can feel restrictive and socially isolating. Going out to eat, traveling, or attending parties can become stressful when you’re constantly worrying about the FODMAP content of your food.
After completing the reintroduction phase, you’ll be able to bring back a wider variety of foods, making it easier to eat out, share meals with friends, and enjoy life—without being worried about gut upset.
-
Long-Term Health Depends on a Varied Diet
A diet that’s too limited can make it hard to get all the nutrients your body needs. Reintroducing tolerated high FODMAP foods helps you:
- Increase fiber intake
- Support gut health
- Ensure nutritional adequacy over time
SUMMARY
Even if you feel great now, the FODMAP reintroduction phase is the key to sustainable, long-term health, symptom management and a happier, more flexible relationship with food.

What Happens When You Find A Food Problematic
The FODMAP reintroduction phase can feel a bit like a roller coaster—exciting, but also a little nerve-wracking. The good news? This phase is where you start to truly understand your body and learn which foods work for you—and which ones don’t.
As you go through the process, you’ll likely discover some high FODMAP groups that your gut can handle (yay!), and it’s also normal to come across a FODMAP group or serving size that can increase gut sensations.
When you react to a challenge food don’t panic
It’s completely normal to experience some degree of symptoms during the reintroduction phase. It doesn’t mean the diet has failed or that you’re back to square one. It just means that your body is giving you valuable feedback.
Remember:
- Symptoms usually settle within 1-3 days. Once the high FODMAP food moves out of your system, your symptoms should return to your baseline, and you can continue with your FODMAP reintroductions.
- You can pause and resume your FODMAP reintroductions at any time. As soon as you start to feel an increase in symptoms during a FODMAP challenge, you can stop and give your gut time to settle.
Finding a trigger is actually a win
Finding a FODMAP group that is involved in your gut symptoms is empowering. Understanding your limits means fewer surprises and a more predictable gut.
You now have clear insight: You’ve confirmed a specific FODMAP or food that your body struggles with.
You can manage your intake: Limit this FODMAP group most of the time, while still enjoying other foods.
Tolerance Can Change Over Time
Just because a food is problematic now doesn’t mean it always will be. FODMAP tolerance can change over time and you can do things to improve your tolerance, so it’s worth retesting foods or FODMAP groups down the road to see if your body responds differently.
SUMMARY
If your gut responds to a FODMAP reintroduction challenge it can be a good thing as it confirms a FODMAP trigger. Remember, symptoms will pass after a few days as the high FODMAP food moves through your system.
Your FODMAP Reintroduction Phase Guide
Before you jump into your FODMAP challenges, there are a few key things you need to know.
FODMAP Reintroduction Success Tips
- Only use a recommended challenge food. A challenge food normally only contains one of the FODMAP groups, so you get clear and accurate results. For example, cow’s milk only contains lactose, while mango only contains excess fructose.
- Understand what normal gut sensations are. A little bit of bloating or gas is a normal. This is a mild gut fluctuation, and doesn’t mean you do not tolerate the challenge. Look out for symptoms that cause significant pain or discomfort and that interrupt your every day life.
- Allow symptoms to settle before starting a challenge. If experience a gut upset with a FODMAP group give yourself three days or until symptoms are settled before you start the next FODMAP challenge.
- Stop the challenge if you get moderate to severe symptoms. These symptoms highlight that you’ve found your threshold level for a FODMAP group. Make sure you make a note of your symptoms, what challenge food you ate, and when they happened.
- Seek expert support. Ideally, work with a FODMAP-trained dietitian or access expert support through our FODMAP Made Easy Program.
FODMAP Challenge Schedules
A challenge schedule is how you space out your FODMAP testing days. Depending on the FODMAP group and your comfort level, there are two main ways to do this.
Challenge Schedule 1: 3 days in a row
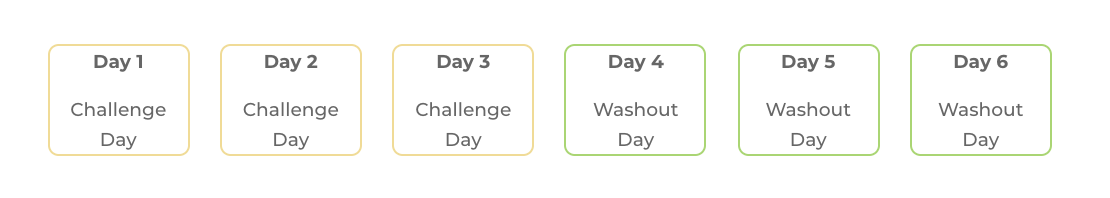
In this schedule, you eat the same challenge food for three days in a row, increasing the portion size each day. You stop the challenge early if you get moderate to severe symptoms. This is a faster method that suits FODMAPs that move quickly through the digestive system, such as lactose, sorbitol, mannitol, and excess fructose.
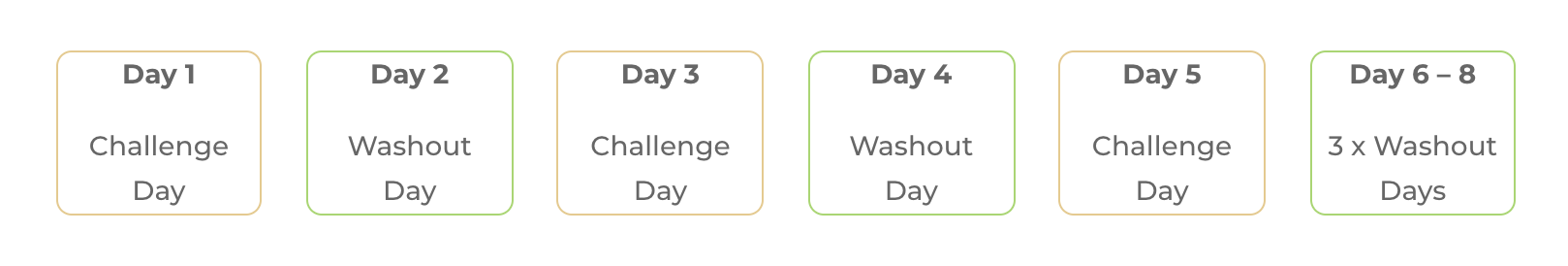
Challenge Schedule 2: Alternate Day Testing (with rest days)
In this challenge schedule, you would eat the challenge food every other day (Day 1, Day 3, Day 5), increasing the serving size each time. On the days in between, rest and monitor symptoms. Stop early if moderate to severe symptoms occur.
This challenge schedule can be good for fructans and GOS, as these FODMAP groups can move more slowly through the gut and are more likely to be involved in a delayed responses (5).
FODMAP Reintroduction Challenge Food Options
Pick your challenge foods based on the FODMAP group you’re testing. These foods should only contain one FODMAP type so you get clear, reliable results.
Here’s a quick cheat sheet:
| FODMAP Group | Challenge Food Example | Serving Suggestions |
| Lactose | Cow’s Milk | ¼ cup, ½ cup, 1 cup |
| Excess Fructose | Orange juice, freshly squeezed | ½ cup, ¾ cup, 1 cup |
| Sorbitol | Fresh Apricot | 2 medium, 3 medium, 4 medium |
| Mannitol | Portobello Mushroom | ⅓ of a mushroom, 1 mushroom, 2 mushroom |
| GOS | Adzuki Beans (canned) | 4 tbsp, 6 tbsp, 8 tbsp |
| Fructan – garlic | Fresh garlic clove | ¼ clove, ½ clove, 1 clove |
| Fructan – onion | White or red onion | 1 tbsp, 2 tbsp, ¼ cup |
| Fructan – fruit & vegetable | Banana, common (ripe – has brown spots) | ½ medium, ¾ medium, 1 medium |
| Sorbitol + Excess Fructose | Apple (green or red) | ¼ apple, ½ apple, 1 apple |
| GOS + Fructans | Pistachio nuts | 8 nuts, 10 nuts, 12 nuts |
Table references: Monash FODMAP, 2025; Monash University FODMAP Diet App
You can access additional challenge food options via your FODMAP trained dietitian, in the Monash University FODMAP Diet App, or via our FODMAP Made Easy program.
Once you have completed your FODMAP Reintroduction challenges you will know what FODMAP groups you can enjoy while keeping your symptoms settled. You can then move from the FODMAP Reintroduction Phase onto a long-term modified low FODMAP diet (also called a personalised low FODMAP diet) where you add high FODMAP foods you tolerate well back into your diet.

Struggling with the Reintroduction Phase? Get Expert Help
You’re not alone — and you don’t have to figure it out by yourself.
The reintroduction phase can be incredibly stressful. Between managing your symptoms, sticking to a low FODMAP baseline, balancing work and social life, and trying to choose the right challenge foods, it’s no wonder many people feel overwhelmed.
That’s exactly why we created the FODMAP Made Easy program — to guide you through this phase with clarity, structure, and support.
Here’s how we’ll help you every step of the way:
- A 12-week, step-by-step online course that tells you exactly what to do each week
- Clear answers to the 10 most commonly asked questions about the reintroduction phase
- A practical guide to help you manage reintroduction anxiety and feel more in control
- Tools to help you create a flexible challenge schedule that fits around your work and social life
- A downloadable success checklist to keep you organised and on track
- A wider selection of challenge foods so you can choose options that suit your taste
- Friendly email support if you have questions or need further support
- A super helpful 15-page downloadable workbook to help you track foods, symptoms, and results
- Support to help you analyse your challenge outcomes and understand what they mean for your diet going forward
You don’t have to keep guessing or going it alone.
Join the FODMAP Made Easy program and get the guidance, support, and tools you need to reintroduce FODMAPs with confidence.
It’s time to take the stress out of this phase and move toward a diet that works for you.

Common FODMAP Reintroduction Mistakes
Still finding challenge foods problematic? Let’s troubleshoot together.
If you’re gut is responding to every FODMAP challenge food, it doesn’t necessarily mean your gut can’t handle any of them. More often than not, it means there might be a few common mistakes getting in the way—or possibly other health conditions that need attention.
Let’s go through the most common reintroduction mistakes and how we can help you move forward with more confidence and clarity.
1. Choosing the wrong challenge foods.
One of the biggest reintroduction mistakes is choosing foods that contain more than one type of FODMAP. This makes it hard to tell which FODMAP is causing the reaction.
For example:
If you’re testing for excess fructose, a pear is a poor choice—it contains both excess fructose and polyols (sorbitol). That mix can confuse your results.
Instead, choose a food that contains only the FODMAP you’re testing. For excess fructose, try mango or freshly squeezed orange juice, which give you a clearer picture of your tolerance.
How we can help:
In the FODMAP Made Easy Program you get instant access to our FODMAP Reintroduction Course that gives additional challenge food options—so there’s no second-guessing.
2. Not following the low FODMAP diet during the challenge.
To get accurate results, you need to keep the rest of your diet strictly low FODMAP while you’re testing challenge foods. That means:
- Only testing one challenge food at a time
- Sticking to low FODMAP meals and portion sizes
- Avoiding high-FODMAP “surprises” in packaged or restaurant foods
This way, if symptoms show up, you’ll know what’s going on: the challenge food.
Also keep in mind:
Some gut irritants like caffeine or alcohol are technically low FODMAP, but can still affect gut symptoms in sensitive individuals. It’s a good idea to limit them on challenge days. If you suspect they’re problematic for you. You can always test them separately later with your dietitian’s support.
How we can help:
Our low FODMAP meal plans, delicious recipes, and expert chat support are all included in the FODMAP Made Easy program. We’ll help you stay on track and confidently incorporate your challenge foods into meals you’ll actually enjoy.
3. Starting with too much of the challenge food.
Another common mistake is starting off with a large portion of the challenge food. If your gut reacts strongly, you might assume you can’t tolerate that FODMAP group at all—when actually, a smaller amount might have been okay.
Here’s how to do it right:
Start small. If your gut feels good, gradually increase the amount over 2–3 days.
For example, don’t begin with a full garlic clove when testing fructans. Start with ¼ clove, then go up to ½, and so on.
This step-by-step approach gives your gut a better chance to adjust—and helps you discover your personal tolerance threshold for the FODMAP group.
How we can help:
We provide recommended portion sizes, tracking tools, and personal support to help you test smarter—not harder. You’ll find everything you need inside the FODMAP Made Easy program.
4. There may be other food sensitivities or health conditions at play
If you’re gut is still responding to every FODMAP challenge—even after following all the right steps, then it’s time to talk with a FODMAP-trained dietitian.
Some people have additional issues that can affect results, including:
- Non-FODMAP food sensitivities (like wheat or food chemicals: salicylates, amines, glutamates, sulphites)
- Small Intestinal Bacterial Overgrowth (SIBO)
- Other digestive or inflammatory conditions
Don’t jump to conclusions on your own. Your dietitian can help you explore these possibilities and guide you through further testing or referrals if needed.
Final Thoughts
The FODMAP Reintroduction phase can feel like one of the most confusing parts of the low FODMAP diet —but it doesn’t have to be. With the right guidance, clear structure, and support along the way, the reintroduction phase becomes a powerful tool for understanding your body and building a diet that actually works for you.
References:
- Mansueto, P., Seidita, A., D’Alcamo, A., Carroccio, A.Role of FODMAPs in Patients with Irritable Bowel Syndrome: A Review. Nutrition in Clinical Practice Journal. 2015-02-18. DOI: 10.1177/0884533615569886. Retrieved from https://aspenjournals.onlinelibrary.wiley.com/doi/abs/10.1177/0884533615569886
- Mullin, G., Shepherd, S., Roland, B., Ireton-Jones, C., & Matarese, L.Irritable Bowel Syndrome: Contemporary Nutrition Management Strategies. Journal of Parenteral & Enteral Nutrition. 2014: Volume 38: Number 7. 781-799. DOI: 10.1177/0148607114545329. Retrieved from https://pubmed.ncbi.nlm.nih.gov/25085503/
- Scarlata, K.Low FODMAP Diet is Not a Forever Diet. Well Balanced. 2014-09-02. Retrieved from:http://blog.katescarlata.com/2014/09/02/low-fodmap-diet-forever-diet/. Retrieved on: 2015-03-21.
- Monash Fodmap Team. Reintroduction Update. Monash University FODMAP Blog. 2025-04-28. Retrieved from https://monashfodmap.com/blog/reintroduction-update/
- Tuck C., & Barret, J. Re-challenging FODMAPs: The low FODMAP diet phase two. Journal of Gastroenterology and Hepatology. 2017: Volume 32: Issue 1, p. 11-15. Doi 10.1111/jgh.13687
- Monash University FODMAP Diet App. Food Guide. The Monash University Low FODMAP Diet App. 2025: 4.0.1(521). Date retrieved: 2025-05-01. Retrieved from: https://monashfodmap.com/ibs-central/i-have-ibs/get-the-app/ Accessed: 2025-05-01
- BPACnz.Irritable bowel syndrome in adults: Not just a gut feeling. Best Practice Journal. 2014: Issue 58. 14-25. Retrieved from http://www.bpac.org.nz/BPJ/2014/February/ibs.aspx
- Gibson, P., Barrett, J. & Muir, J.Functional bowel symptoms and diet.Internal Medicine Journal. 2013: Issue 42. 1067-1074. DOI:10.1111/imj.12266. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/24134168
- Varney, J. Practical Tips For FODMAP Reintroduction. Monash University FODMAP Blog. 2020-01-06. Retrieved from: https://monashfodmap.com/blog/practical-tips-fodmap-reintroduction/ Retrieved on 2025-05-
Image credit: All Kind of People/Shutterstock.com












So far it is working great!
Hi Kathy,
It’s great to hear you are success reintroducing FODMAPs. Keep up the good work!
I’m grateful for your site. Trying to navigate all this alone would be very difficult. You give great resources and positive outcomes. Thank you!!
Hey Alana,
Thanks so much for this incredibly detailed page!
Does this mean you can pick one of the suggested fodmap foods (i.e. avocado) and slowly move from the small dose to the larger recommended dose over a week long period (utilising one of the above time tables) to test the whole food group? Once this is completed/if you have no symptoms does this mean you can reintroduce other things from that group? It’s hard to know because the portion sizes of different foods within that group will obviously vary.
Thanks heaps!
I sure wish you had a reply, because it’s an important question and I’d like to know the answer too. If I don’t react to a fodmap in one food, does that automatically mean that all other foods with that single fodmap are okay for me too?
Hi Kate,
If you don’t react to the FODMAP challenge food then that is a good indicator that you should tolerate other foods containing that FODMAP group well. The one exception is fructans. When you challenge fructans we do recommend that you do several challenges, as sometimes you can react to different fructan containing foods differently. I hope that helps!
Hi there,
I am about to start the reintroduction phase and I am a little bit confused. When researching what I could eat during the elimination phase I found that leeks were low-fodmap friendly and so were chickpeas if no more than 1/4 cup eaten. So why are these foods in the reintroduction phase?
Hi Stephanie,
Only the green leaves of the leek are low FODMAP. The white bulb is high FODMAP for fructans. This means the leek bulb can be used during the re-challenge tests to check your tolerance to fructans.
In terms of chickpeas, only canned chickpeas are low FODMAP in 1/4 cup serves and then they become high FODMAP in larger serves. This means dried chickpeas can be used to check your tolerance levels. You can also use canned chickpeas providing you use a serving size larger than 1/4 cup. Does that help?
Hi,
Thanks for all the great info!
Just one quick question: when it says to test two foods from a single reintroduction group, address those tested simultaneously or separately? E.g. Do I test garlic and onions tested together at recommended amounts, or reintroduce garlic one week and do onions the following week?
I would so appreciate any clarification you could provide! Thanks!
Hi Alexandra,
We would recommend you split onion and garlic into two separate tests over two weeks. For example, do garlic one week and onion the next. If you need more reintroduction support we have a 12-week reintroduction e-course that walks you through each of the FODMAP challenges and gives you lots of tips along the way. You can find the e-course in our Wellness Club: https://app.alittlebityummy.com/dashboard
Hi Alana,
If I have a reaction two days after testing the last group, during washout period, do I attribute that to the last food group tested? I had a mild reaction to lactose which seems to have become slightly worse 2 days after the last day of testing. Should I go onto the next group tomorrow or wait for the symptoms to subside?
Thanks,
Lino
Hi Lino,
We would recommend that you wait for symptoms to subside before moving onto the next FODMAP challenge. Also it isn’t normal to react two days later (generally reactions start within 24 hours). This means at the end of your FODMAP challenges we would suggest you test that group again and see if you get the same results. Does that make sense?
Yes, completely !
Thanks for the information and your site. Very useful. L
Do you have to reintroduce the foods in the order they are listed or can you do any order your choose? For instance I’d love to try garlic first, is that OK?
Hi Brooke,
You can do the challenges in whatever order you want! Just make sure you leave at 3 washout days between each challenge so you get clear results. All the best with your garlic challenge!
What is a wash out day on the reintroduction phase of the diet?
Hi Cammy,
A washout day is where you go back to only eating low FODMAP foods. These washout days help you settle any symptoms from the previous food challenge so that you get clear results from your next challenge test.
I’m now on my last reintroduction (blackberries) and it will be a relief to finally finish what has been a 12 week long, tedious but very interesting series of tests.
Along the way I struggled with the bread but found in UK supermarkets the Schar seeded ciabattas were about the tastiest thing. I also found it a minefield but my dietician suggested I download the Monash FODMAP app onto my iPhone and you can scan the bar codes on the products and the app will tell you if it is suitable to eat or not. It is a bit over sensitive with flavourings but other than that brilliant and saved me a lot of time and effort.
I had no major reactions until I tested Polyol Mannitol with celery and I had diarrhoea on day three before I ate that days celery and the next day I was ok. I suffer from slow colon transit constipation so I’m wondering if I can use celery when I’m very bunged up to go to the loo or is that not really the point?
Alana, would you be able to help with this please?
My last challenge was GOS and I tested with 15 almonds, within an hour I looked like I had swallowed a ball and felt awful all day. Day 2 20 almonds, I didn’t feel too bad but Day 3 of 30 almonds made me feel like an absolute slug but the next day I was ok and glad to be in the washout period!
Alana, does this mean I could eat a small amount of hummus ?
I finish the reintroduction on Saturday and I want to have a cream cheese and marmite sandwich on squidgy white bread!
The most pleasurable reintroduction was onion .. OMG I made a basic pasta sauce with prawns, tomato and basil with onion and never realised just how much flavour onion gives a dish, it was delicious.
I also felt like Charlie finding the Golden Ticket in the Wonka Bar when I scanned the barcode of a pack of strawberry Fruitellas to find I could eat those after four months they tasted like heaven! Small pleasures are the thing that got me through the diet. Good luck to everyone who is on the diet!
Emma
Hi Emma,
Thanks for commenting! The Monash App doesn’t have a bar code scanner so did you mean the FoodMaestro FODMAP app? I’m glad it helped you find a few more foods to eat.
The reintroduction phase can often help you find the right balance for your long term diet. Some of the FODMAPs, like mannitol, act like natural laxatives and can help you stay regular. This means you can definitely incorporate them into your diet as needed and it sounds like using the day 1 challenge dose might be a good place to start. There is also some more information provided in here: https://alittlebityummy.com/can-reintroducing-fodmaps-help-reduce-constipation/
Your almond reaction is intriguing. FODMAP reactions take place in the large intestine so a reaction after an hour for a solid food like almonds is unusual. I would suggest your retest GOS using chickpeas instead and see if you get the same reaction. Also it’s good to note that you can make low FODMAP hummus and enjoy a small amount. Here is a recipe: https://alittlebityummy.com/recipe/en-us/traditional-low-fodmap-hummus/
Also congratulations on getting onion back! That will give you a huge amount of food freedom especially when you are eating. I hope my answers help and just let me know if you have more questions.
Thank you so much for this, your whole website has been brilliant. I have looked at lots of different sites and started my diet off with a qualified dietician who didn’t explain things nearly as well as you have.
Sorry, yes you are correct it was the Food Maestro app I used and I did find it useful.
I finished the whole diet yesterday and I will, as you suggest, retake the GOS test with chickpea as I had just started on HRT and had a lot of stress at home at the time of that test.
I just finished the Sorbital reintroduction using Blackberries (2, 5, 10 blackberries three days) and it had the complete opposite effect to what I expected and gave me terrible constipation.
I’m really glad I have finished, I only had symptoms for GOS, Sorbital and Mannitol. I would really like to learn how to manage that as I don’t currently know what all the foods are in each group. Can I buy your book on Amazon please?
Thanks again, you really have helped me a lot.
Emma
Hi Alana,
If I want to introduce sorbitol, but fresh apricots aren’t in season yet and I dislike cherries, what would you recommend I use for the reintroduction phase?
Hi Gemma,
We would normally recommend breath mints that have sorbitol as their main sweetener. We talk about how to use these for a sorbitol challenge in the FODMAP Made Easy program.
I’ve gone through all the challenges without any problems – does that meanIi probably didn’t/don’t have IBS but some similar condition symptoms-wise? Nothing came from my doctors tests either…
Hi Phil,
It’s great to hear that you have passed all the FODMAP challenges and can regain your food freedom. This doesn’t mean you don’t have IBS, it just means that FODMAPs aren’t the cause of your symptoms. If you think your symptoms are still food-related then now is a good time to talk to a dietitian who has specialised in gut conditions about other potential trigger foods. Otherwise looking at non-food treatment strategies could be a good next step. These could include cognitive behavioural therapy, gut hypnotherapy, or even stress/anxiety strategies like yoga or meditation.
When challenging garlic does it matter of it’s cooked or raw?
Hi Sara,
You can use raw or cooked garlic for your challenge. We suggest you look at how you normally eat it and then challenge the garlic that way. I hope that helps!
I just completed the fructose test on honey and passed it but does that mean I passed all fructose or just honey? Do I keep to test everything from every group or just one thing from every group? This can be so confusing sometimes
Hi Hayley,
For most of the FODMAP groups if you pass the challenge using one food you should tolerate the other foods in the same group too. This means you should tolerate all foods containing excess fructose (providing they don’t also include another FODMAP group).
Fructans are the exception. With this FODMAP group we normally recommend doing 3 challenges – wheat base challenge, onion challenge and garlic challenge as we find people often tolerate them differently.
Hi,
I feel very fortunate to have found this website, as all I got from my doctor was a list of foods I could eat and those I should avoid, and a very vague explanation of the process of reintroducing those foods.
I have been following the strict elimination phase for three weeks, and I feel great. Until I got to your very detailed explanation, I believed that once I tested a food and tolerated it, I could include it on the rest of the reintroduction phase. That is clearly not so.
My dilemma is this — my niece is studying abroad this semester in Rome, and I will visit her the week of Thanksgiving. Having put three weeks into this already, I hardly want to throw my efforts away, but on the other hand, I do not want to spend a week in Italy turning down most of the food and being the one who has to ask for specially prepared food at every meal. What do I do?
I thought I could try reintroducing wheat, garlic, and onion, in particular, and then know whether or not I could have those on my trip, but that is not how the “challenges” are supposed to work. Any advice?
If I eat things that are not low FODMAP on the trip, and have to start over when I get back, how long would I then have to wait before starting the challenges? I did wonder if I should have waited until after the trip to even start, but honestly, even if I have to do it all again, the improvement in my symptoms has been worth the sacrifices these three weeks.
I really appreciate any advice you can give. Thank you!
Hi Stephanie,
Okay so if you have already tested some FODMAP groups and found you can tolerate them, then you can eat those while you are on holiday. When you return from holiday, remove those high FODMAP foods from your diet and go back on a strict low FODMAP diet for 3 days (just like you do after a food challenge). Once your symptoms are settled you can continue testing the FODMAP groups. You don’t have to start the elimination phase again. I hope that helps!
Hi Alana,
First, thanks for the good advice regarding my trip to Italy. I was able to enjoy my time there with minimal symptoms, and I went strictly low FODMAP when I returned, as you suggested, before getting back to the testing.
I have another question now, and forgive me that it is a bit of a TMI, but I need to ask about gastrointestinal issues getting worse around the time of my period. Yesterday I had a rough day symptom-wise, and I was testing a new food group, but it was also the first day of my period. I am not sure I can attribute the issues to the food, or if they are just the effects of my hormonal fluctuations. My idea was to stop this challenge now and then try retesting the same food at a different time. With all the people who write to you, has anyone had this question? I tried searching your blogs and did not find anything on this topic. Thank you!
Hi Stephanie,
Thanks for commenting! It’s awesome to hear that you had a great time in Italy. In answer to your question – yes it is really normal for hormonal swings to influence symptoms. Joanna Baker, one of our dietitian team has a great article on this topic: https://everydaynutrition.com.au/does-your-period-make-ibs-worse/
Your idea is also right. Stop the challenge, allow the symptoms to settle and then reset the same food when you are on your period. I hope that helps and that you feel better soon.
Do you have suggestions on how to reintroduce Garlic and Onion? I don’t really want to sit down and eat a clove of garlic or half an onion. I could eat foods that contain these items but then I won’t really know how much I am eating. Is there a recipe I should use or any other suggestions?
Hi Jennifer,
We recommend measuring out the amount of onion/garlic you need to eat for your challenge, pan fry it, and then mix it through your meal. That way you can enjoy it a meal (like a salad, burger, spaghetti bolognese, pasta dish or stir-fry) and don’t need to sit down and eat it by itself.
Hi Alana,
first of all thank you very much for your good help with all this precious information.
My question is: after challenging a food without symptoms, can I continue eating this food (or food group) during the next challenging food groups?
Thanks
Hi Ana,
That is a great question. Even if you pass a challenge, we suggest leaving that FODMAP group out of your diet until you finish your other challenges. Sometime FODMAPs can build up in our system. This means you might be fine with several FODMAP groups when you eat them separately but have issues when you combine them. That means it’s important to challenge each group by itself first.
Hi Alana,
Thank you for this FODMAP reintroduction guide, it’s a great help!
My question is, if I am also on a gluten-free diet, how can I test for Fructans containing grains?
Thank you
Hi Jack,
So you have a couple of options here. Instead, you could do an inulin challenge and see how you go eating rice crackers that contain inulin or chicory root as an ingredient. Alternatively you could use gluten free couscous made from rice and corn – start with 1/3 cup and work your way up to 1 cup cooked.
If I was going to test using GF rice crackers, what would you suggest using as the 3 day test challenge amounts? Is it okay if the crackers have both inulin and chicory root or should I try to buy ones that only have 1 of the 2 ingredients?
Hi Cara,
Inulin is usually derived from chicory root and it can be labelled on ingredient labels as inulin, chicory root, chicory root fibre. That means it’s okay if the ingredient list states both. We hope that helps.
can you take a break mid-reintroduction phase (ie. for a surgery and recovery) and then resume re-introduction phase after recovery all the while maintaining a low-fodmap diet including the foods that have been reintroduced successfully followed by a 3 day washout after recovery?
Hi Katrina,
Thanks for commenting.Yes you can pause the reintroduction phase if you need to. Just make sure you give yourself three washout/rest days where you don’t eat high FODMAP foods before you pick up your FODMAP reintroductions again.
Also, remember that high FODMAP foods that you’ve passed should remain out of your diet while you finish the other reintroductions.
Hello,
I’ve made it a few weeks into the reintroduction phase. Regarding bringing back in onion and garlic, should it be cooked (or raw) onion or garlic in a dish rather than onion/garlic powder or juice in a condiment or cracker, etc?
Hi Kile,
That is a great question. We suggest you start with cooked or raw onion or garlic in a dish first as this will give you a lot more options when eating out. Then try a product that has onion or garlic powder in it.
So, I made it to the very last challenge without much in the way of symptom exacerbation. But the apple challenge seems to be a problem. How do I use this information as I loosen up restrictions as apples have fructose plus sorbitol?
Confusing since mango and blueberries were fine. Thank you
Hi Sharon,
It’s awesome to hear that you passed the individual FODMAP group challenges without too much issue. This shows that you can tolerate the FODMAP groups by themselves well. Your reaction to apples shows that your gut issues might be related to combining FODMAP groups by either having a food that has two FODMAPs in it OR by having a meal with several ingredients that have different high FODMAP groups. When you combine the FODMAPs you are going over your tolerance level and triggering your symptoms. As you relax your diet start by just having 1 high FODMAP group in a meal (eg honey for excess fructose). Over time you can experiment with different FODMAP combinations over the course of a day or a meal. Does that help?
I seem to be able to tolerate sorbitol and fructose just fine separately, but struggle with them combined. For instance, I don’t have a problem with avocado, blackberries, or honey, but a whole apple sets me off. Is this normal?
Hi Lindsay,
Thanks for commenting. This can be really common and is linked to FODMAP stacking. This issue is also why it’s recommended that you test each FODMAP group individually while keeping the rest of your diet low FODMAP.
Hello! I just tested wheat, garlic and onions separately and found that wheat was ok but onions and garlic aren’t. Does this mean I should be ok with other fructans (like broccoli and asparagus, for example?) How can I know what should be ok on the list of frutans when my reaction differed with the three tests? Thanks so much for all this help! Your articles are incredibly helpful.
Well done on pushing through your FODMAP reintroductions. You can definitely do a reintroduction for fructan containing vegetables. Broccoli isn’t a good choice for testing as you have to eat a lot of it to reach a high fructan amount (4 cups in one serving). Asparagus contains both fructans and fructose so we wouldn’t use that either.
Instead we would suggest: globe artichoke, brussel sprouts, savoy cabbage, zucchini/courgette.
– Globe artichokes – start with 1/8 small globe artichoke and work your way up to 1 whole small globe artichoke.
– Brussel sprouts – start with 3 sprouts and work your way up to 6 sprouts
– Savoy cabbage – start with 3/4 cup and work your way up to 1.5 cups
– Courgette/Zucchini – start with 75g and work your way up to 100g
Hi , Can u tell me if only one food needs to be eaten that we are testing for our tolerance level or multiple high fodmap food can be eaten together though in low amount like in day one, then increasing amount on day 2 of similar multiple high fodmap food
Hi Sarvesh,
For each reintroduction challenge we suggest picking one high FODMAP food to challenge with and keeping that consistent for each challenge day (make sure the rest of your food is low FODMAP). On each test day you then increase the amount you have. You are testing the FODMAP in the food, not the food itself so generally you only need to test one food per FODMAP group. The exception here is fructans where we recommend you do a fructan grain challenge, an onion challenge, an garlic challenge.
Hello,
I am confused by the quantities during reintroduction: are these quantities in a meal or is it spread out throughout the day? For example, having a 1/2 onion in one single meal seems like a lot to me. Could that be spread out during the day among multiple meals?
Hi Erica,
Thanks for commenting. Ideally, you want to eat the challenge food amount in one sitting as it’s the level of FODMAPs in the food you are testing not the food itself. Just remember that FODMAP challenges can be tailored to your personal needs that means you can reduce or increase the last test day amount to the largest amount of the food you would normally eat. We hope that helps.
That is very helpful! Thank you!
Hi Erica,
You are welcome! It’s lovely to hear you are finding the article helpful.
This is soooo helpful thank you!! I am trying to plan my reintroduction phase using this info and the monash app. I’m a bit confused about the galactans/GOS challenge as the challenge foods also have fructans eg chickpeas. Please can you recommend something that only has GOS which I can try? Or is the point that I’m testing both together – in which case should I do fructans by itself first (I’m pretty sure this is an issue for me)?
I also wanted to check if it’s ok to take a break every few weeks and enjoy having foods I’ve found I can tolerate – as a kind of reward and encouragement to keep going. Reading the comments, this looks fine as long as I do a washout for 3 days afterwards and go back to the low fodmap diet while I’m doing the rest of the challenges. Is that right?
Thanks so much!!
Hi Sarah,
Thanks for commenting. Canned chickpeas and sprouted chickpeas only contain GOS according to Monash University. Lots of people also use almonds to test GOS. You can definitely test fructans first – just remember that people tolerate different fructan groups differently so make sure you do all of the different challenges.
You can also take a break between challenges if you want to. Our recommendation would be to have 3 washout days and make sure symptoms are settled before you restart.
I am nearing the end of reintroductions and my issues are always the morning following (extreme rumbling and diarrhea) . However, when confidently not having issues on last day of reintroduction (or the other days after introducing the food) I am wondering if skipping the washout day is suitable or can I do the next challenge food if confident I had no issues. I am also a dietitian so this has been a great learning for me to actually do the diet and learn.
Hi Connie,
Thanks for commenting. As your symptoms appear the next day, we suggest leaving 24 hours between starting a new food reintroduction challenge just so you can be fully confident of your tolerance levels (you don’t have to do a full three day washout/rest period). We hope that helps!
Thank you so much for this article. I have a question:
TLDR: I’m part way through the reintroduction phase – can I take a break from strictly following fodmap while on holiday without having to restart from the elimination phase?
I’m so excited to be going on holiday to France in a few days! I would love to be able to take a break from strictly following fodmap for the week so I can eat some delicious food and eat out more easily. I am prepared to deal with any resulting symptoms – I am lucky my IBS is not severe. However, I don’t want to lose all the hard work of the past few months (I’m a few weeks into testing/reintroducing – so far only sorbitol has given me any trouble). I would like to know if breaking from fodmap now will mean I have to do another whole elimination phase on return before I can resume the reintroduction phase. If not – fingers crossed! – how long a ‘wash out’/reset phase of strict fodmap should I do before going back to testing?
TIA!
Hi Lu,
That is a great question! You won’t undo all your hard work by having a break from the low FODMAP diet while you are on holiday. When you return go back on the low FODMAP diet for 3-5 days to give any symptoms a chance to settle, then you can pick up your FODMAP reintroduction challenges from where you left off.
Thank you for your fantastic website! Two questions (before I start): is there a less intense way to test some challenging FODMAP groups, without doing the whole elimination and re-introduction? Secondly, is there a recommended order of FODMAPs to re-introduce to give the best outcome?
Hi Vanessa,
Thanks for commenting. Instead of doing a full low FODMAP phase you can do a simplified low FODMAP diet instead. We have resources on how to do this in our FODMAP Made Easy program. In this program, we can also help you change challenge schedules and the order of the reintroductions to best suit your needs. You also have full email support to help answer your questions: https://alittlebityummy.com/fodmap-made-easy/